Nitrodilators and Soluble Guanylyl Cyclase Activators
General Pharmacology — Nitrodilators
Nitric oxide (NO), a molecule produced by many cells in the body, and has several important actions (click here for details). In the cardiovascular system, NO is primarily produced by vascular endothelial cells. This endothelial-derived NO has several important functions, including relaxing vascular smooth muscle (vasodilation), inhibiting platelet aggregation (anti-thrombotic), and inhibiting leukocyte-endothelial interactions (anti-inflammatory). These actions involve NO-stimulated formation of cGMP. Nitrodilators are drugs that mimic the actions of endogenous NO by releasing NO or forming NO within tissues. These drugs act directly on the vascular smooth muscle to cause relaxation and therefore serve as endothelial-independent vasodilators.
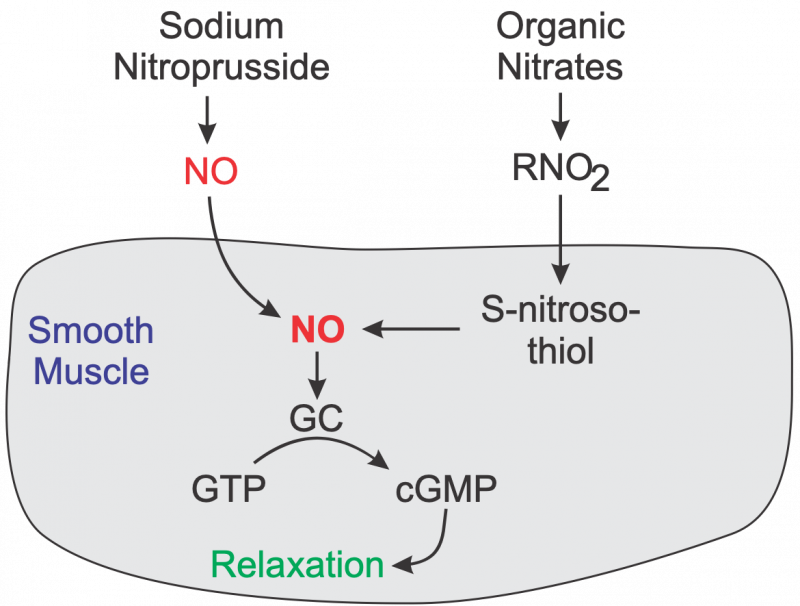 There are two basic types of nitrodilators: those that release NO spontaneously (e.g., sodium nitroprusside) and organic nitrates that require an enzymatic process to generate NO. Organic nitrates do not directly release NO, however, their nitrate groups interact with enzymes and intracellular sulfhydryl groups that reduce the nitrate groups to NO or to S-nitrosothiol, which then is reduced to NO. Nitric oxide activates smooth muscle soluble guanylyl cyclase (GC) to form cGMP. Increased intracellular cGMP inhibits calcium entry into the cell, decreasing intracellular calcium concentrations and causing smooth muscle relaxation (click here for details). NO also activates K+ channels, which leads to hyperpolarization and relaxation. Finally, NO acting through cGMP can stimulate a cGMP-dependent protein kinase that activates myosin light chain phosphatase, the enzyme that dephosphorylates myosin light chains, which leads to relaxation.
There are two basic types of nitrodilators: those that release NO spontaneously (e.g., sodium nitroprusside) and organic nitrates that require an enzymatic process to generate NO. Organic nitrates do not directly release NO, however, their nitrate groups interact with enzymes and intracellular sulfhydryl groups that reduce the nitrate groups to NO or to S-nitrosothiol, which then is reduced to NO. Nitric oxide activates smooth muscle soluble guanylyl cyclase (GC) to form cGMP. Increased intracellular cGMP inhibits calcium entry into the cell, decreasing intracellular calcium concentrations and causing smooth muscle relaxation (click here for details). NO also activates K+ channels, which leads to hyperpolarization and relaxation. Finally, NO acting through cGMP can stimulate a cGMP-dependent protein kinase that activates myosin light chain phosphatase, the enzyme that dephosphorylates myosin light chains, which leads to relaxation.
Tolerance to organic nitrates occurs with frequent dosing, which decreases their efficacy. The problem is partially circumvented by using the smallest effective dose of the compound, coupled with infrequent or irregular dosing. The mechanism for tolerance is not fully understood, but it may involve depletion of tissue sulfhydryl groups, or scavenging of NO by superoxide anion and the subsequent production of peroxynitrite that may inhibit guanylyl cyclase.
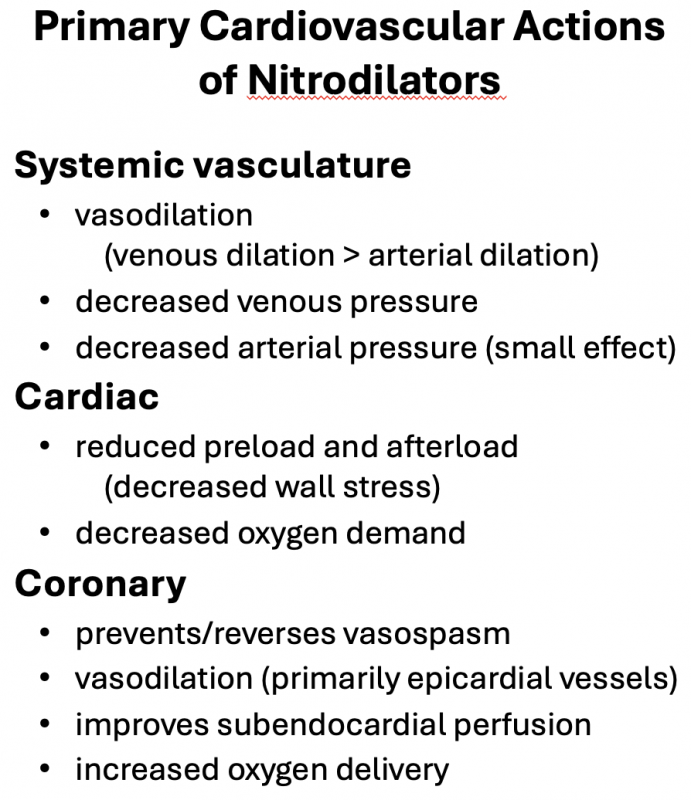 Although organic nitrates can dilate both arteries and veins, venous dilation predominates when these drugs are given at normal therapeutic doses. Venous dilation reduces venous pressure and decreases ventricular preload. This reduces ventricular wall stress and oxygen demand by the heart, enhancing the oxygen supply/demand ratio. A reduction in preload (reduced diastolic wall stress) also helps to improve subendocardial blood flow, which is often compromised in coronary artery disease. Mild coronary dilation or reversal of coronary vasospasm will further enhance the oxygen supply/demand ratio and diminish the anginal pain. Coronary dilation occurs primarily in the large epicardial vessels, which diminishes the likelihood of coronary vascular steal. Systemic arterial dilation reduces afterload, which can enhance cardiac output while reducing ventricular wall stress and oxygen demand. At high concentrations, excessive systemic vasodilation may lead to hypotension and a baroreceptor reflex that produces tachycardia. When this occurs, the beneficial effects on the oxygen supply/demand ratio are partially offset. Tachycardia, by reducing the duration of diastole, decreases the time available for coronary perfusion, most of which occurs during diastole (click here for more details).
Although organic nitrates can dilate both arteries and veins, venous dilation predominates when these drugs are given at normal therapeutic doses. Venous dilation reduces venous pressure and decreases ventricular preload. This reduces ventricular wall stress and oxygen demand by the heart, enhancing the oxygen supply/demand ratio. A reduction in preload (reduced diastolic wall stress) also helps to improve subendocardial blood flow, which is often compromised in coronary artery disease. Mild coronary dilation or reversal of coronary vasospasm will further enhance the oxygen supply/demand ratio and diminish the anginal pain. Coronary dilation occurs primarily in the large epicardial vessels, which diminishes the likelihood of coronary vascular steal. Systemic arterial dilation reduces afterload, which can enhance cardiac output while reducing ventricular wall stress and oxygen demand. At high concentrations, excessive systemic vasodilation may lead to hypotension and a baroreceptor reflex that produces tachycardia. When this occurs, the beneficial effects on the oxygen supply/demand ratio are partially offset. Tachycardia, by reducing the duration of diastole, decreases the time available for coronary perfusion, most of which occurs during diastole (click here for more details).
Therapeutic Indications
The primary pharmacologic action of nitrodilators, arterial and venous dilation, makes these compounds useful in the treatment of hypertension, heart failure, angina and myocardial infarction. Another beneficial action of nitrodilators is their ability to inhibit platelet aggregation.
Hypertension
Nitrodilators are not used to treat chronic primary or secondary hypertension; however, sodium nitroprusside and nitroglycerin are used to lower blood pressure in acute hypertensive emergencies that may result from a pheochromocytoma, renal artery stenosis, aortic dissection, etc. Nitrodilators may also be used during surgery to control arterial pressure within desired limits.
Heart failure
Nitrodilators are used in acute heart failure and in severe chronic heart failure. Arterial dilation reduces afterload on the failing ventricle and leads to an increase in stroke volume and ejection fraction. Venous dilation reduces venous pressure, which helps to reduce edema. Reducing both afterload and preload on the heart also helps to improve the mechanical efficiency of dilated hearts and to reduce wall stress and the oxygen demands placed on the failing heart.
Angina and myocardial infarction
Organic nitrates are used extensively to treat angina and myocardial infarction. They are useful in Printzmetal's variant angina because they improve coronary blood flow (i.e., increase oxygen supply) by reversing and inhibiting coronary vasospasm. They are important in other forms of angina because they reduce the preload on the heart by producing venous dilation, which decreases myocardial oxygen demand. It is unclear if direct dilation of epicardial coronary arteries plays a role in the antianginal effects of nitrodilators in chronic stable or unstable angina. These drugs also reduce systemic vascular resistance (depending on dose) and arterial pressure, which further reduces myocardial oxygen demand. Taken together, these two actions dramatically improve the oxygen supply/demand ratio and reduce anginal pain.
Specific Drugs
The following nitrodilators are commonly used in the USA:
- nitroglycerin
- isosorbide dinitrate
- isosorbide mononitrate
- sodium nitroprusside
The nitrodilators listed above differ in the route of administration, onset of action, and duration of action. Nitroglycerin, which has been used since the 19th century, is commonly used in the treatment of angina because it is fast acting (within 2 to 5 minutes) when administered sublingually. Its effects usually wear off within 30 minutes. Therefore, nitroglycerin is useful for preventing or ending an acute anginal attack. Longer-acting preparations of nitroglycerin (e.g., transdermal patches) have a longer onset of action (30 to 60 minutes), but are effective for 12 to 24 hours. Intravenous nitroglycerin is used in the hospital setting for unstable angina and acute heart failure.
Isosorbide dinitrate and mononitrate, and tetranitrate compounds have a longer onset of action and duration of action than nitroglycerin. This makes these compounds more useful than short-acting nitroglycerin for the long-term prophylaxis and management of coronary artery disease. Oral bioavailability of many organic nitrates is low because of first-pass metabolism by the liver. Isosorbide mononitrate, which has nearly 100% bioavailability, is the exception. Therefore, oral administration of these compounds requires much higher doses than sublingual administration, which is not subject to first-pass hepatic metabolism.
The metabolites of organic nitrates are biologically active and have a longer half-life than the parent compound. Therefore, the metabolites contribute significantly to the therapeutic activity of the compound.
Sodium nitroprusside, unlike organic nitrates, dilates arterial resistance vessels more than venous vessels. Because of its rapid onset of action, it is used to treat severe hypertensive emergencies and severe heart failure. It is only available as an intravenous preparation, and because of its short half-life, continuous infusion is required.
Pharmacology of Soluble Guanylyl Cyclase Stimulators
A new class of drugs, soluble guanylyl cyclase (sGC) stimulators, directly activates sGC to produce cGMP. As described above, sGC is the enzyme that is activated by nitric oxide and nitrodilators to form cGMP, which produces vasodilation. By directly activating sGC, sGC stimulators mimic the effects of nitrodilators. Riociguat is approved for treatment of pulmonary arterial hypertension by functioning as a pulmonary arterial vasodilator. This drug is orally active and can be administered up to three-times daily.
Side Effects and Contraindications
The most common side effects of nitrodilators are headache (caused by cerebral vasodilation) and cutaneous flushing. Other side effects include postural hypotension and reflex tachycardia. Excessive hypotension and tachycardia can worsen the angina by increasing oxygen demand. Prolonged use of sodium nitroprusside carries the risk of thiocyanate toxicity because nitroprusside releases cyanide along with NO. The thiocyanate is formed in the liver from the reduction of cyanide by a sulfhydryl donor. There is clinical evidence that nitrodilators may interact adversely with cGMP-dependent phosphodiesterase inhibitors that are used to treat erectile dysfunction (e.g., sildenafil [Viagra®]). The reason for this adverse reaction is that nitrodilators stimulate cGMP production and drugs like sildenafil inhibit cGMP degradation. When combined, these two drug classes potentiate cGMP levels, which can lead to hypotension and impaired coronary perfusion. Because riociguat activates sGC, it should not be administered along with nitroglycerin or PDE5 inhibitors because significant hypotension can occur related to excessive formation of cGMP.
Revised 01/26/2024
 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)